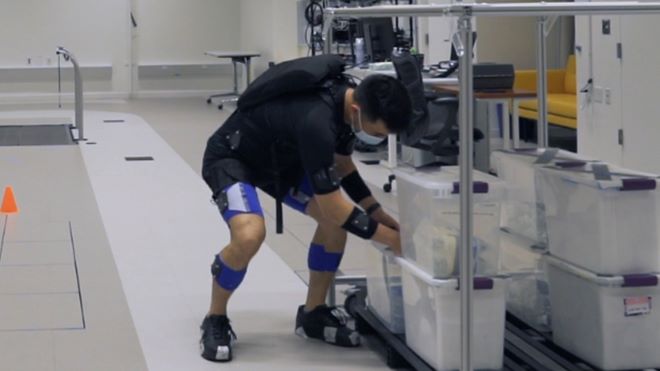
Image credit: Conor Walsh, Harvard Biodesign Lab
Workers lift heavy boxes in a warehouse all day. Office workers and students crouch at their desks for hours. Nurses bend over patients to care for them, and weekend warriors overdo exercise.
Modern life is hard on our backs.
For more than one in four U.S. adults, chronic back pain keeps them from work and enjoying normal activities. Although back pain is incredibly common, its causes and contributing factors differ for every individual. Not only muscles and bones contribute to pain: mood, social situations, physical activity, tissue damage, and other factors also play a role. That’s why back pain is so challenging to treat and why the Back Pain Consortium (BACPAC) Research Program funded by the Helping to End Addiction Long-term® Initiative, or NIH HEAL Initiative®, is looking broadly at a wide range of individual drivers of back pain. The goal is to develop effective, personalized therapies for chronic low back pain that minimize the use of opioids as well as to find ways to help people avoid chronic back pain in the first place.
Researchers in the BACPAC program are tackling this major health problem from a variety of angles, including virtual reality, treating concurrent anxiety, as well as bioengineering approaches such as a wearable device that may help prevent and treat chronic low back pain.
Chronic Low Back Pain Is a Complex Problem
Back pain may start when the spine and muscles are overexerted. Imagine workers in a warehouse moving 30-pound boxes. Over the course of a day, they may lift more than a thousand boxes, and back muscles help lift those thousands of pounds. The muscles eventually tire and can no longer support the spine properly, potentially resulting in strain to muscles and other surrounding tissues, which can lead to low back pain.
To make matters worse, it’s natural to move differently when experiencing pain to minimize discomfort. Because the activity of all our muscles is usually finely coordinated, these avoidance movements can further interfere with normal muscle function and ultimately increase pain. Psychological and social factors, such as feeling anxious, depressed, or stressed, can also make things worse.
Clinical guidelines for low back pain recommend nonpharmacological treatments (like exercise therapy, mindfulness, and learning pain coping skills) along with nonsteroidal anti-inflammatory drugs (like ibuprofen) and antidepressants. However, physical therapists and other healthcare providers working with people who are at risk for back pain – or who are already experiencing it – are looking for more options to help people avoid debilitating pain and to recover faster.
Technology is one solution.
“Artificial Muscle” Helps Support the Back
HEAL-funded researcher Conor Walsh, Ph.D., and his team at the Harvard Biodesign Lab specialize in developing soft “exosuits” – wearable devices that help people with muscle weakness (for example, after a stroke) so they can regain movement and muscle strength. Sort of like Ironman, but with a lightweight suit made of a special fabric that supports specific parts of the body.
Together with physical therapist researcher Diane Dalton, D.P.T., and Lou Awad, Ph.D, D.P.T., from Boston University, Walsh is turning his attention to chronic low back pain. He and his team designed an exosuit consisting of wide fabric straps that run from the shoulders to the thighs. The straps contain sensors that monitor how a person is moving, as well as a motor that can increase or decrease the amount of tension in the straps.
Because the straps are light and flexible, the wearer can move normally while receiving necessary support for each movement. For example, when a person takes a deep squat to pick up a box or object, the motor automatically tightens the straps to provide strong support. But when a person performs a shallower bend or lifts a lighter object, less tension is applied.
The result is that back muscles need to work a lot less. For example, a person wearing the exosuit’s back muscle activity level lifting a weight of 13 pounds without the exosuit was the same as when lifting 22 pounds with it on. For people who perform a lot of heavy lifting, this may make a difference in long-term effects on their back muscles.
Led by postdoctoral fellow David Adam Quirk, Ph.D., the team is now testing the device in a real-world setting with workers whose jobs involve frequent physically strenuous tasks. Half the participants will wear the exosuit during work; the other half will not. Then, after 6 to 8 months, the researchers will compare how often workers in both groups experience back pain and whether those wearing the exosuit have fewer doctor’s visits or days of missed work.
In addition, the research team also plans to soon test the exosuit in people with back pain who are receiving physical therapy. The level of support the exosuit provides is adjustable and can be gradually scaled down as strength and function improve. Over time, the individual should be able to perform movements more on their own, without relying on the extra support.
“We know that the best care for people with back pain is to get them moving as quickly as possible,” Dalton explains. “We think that with the exosuit, they will be able to do more activities earlier and make quicker progress.”
One Piece of the BACPAC Puzzle
Walsh’s exosuit is only one example of how innovative technology can complement currently available nonpharmacological and medication-based strategies to address the problem of chronic low back pain and its treatment. The BACPAC program currently funds over a dozen research projects seeking solutions for the millions of Americans with chronic low back pain.
HEAL-funded researchers are also working to make sure that effective treatments actually reach the people who need them and make a difference. Some of these efforts assess how complementary and integrative approaches like mindfulness training or acupuncture for chronic low back pain can be incorporated into clinical practice. Others are exploring phone-based interventions to help individuals with chronic low back pain who have limited access to in-person healthcare. Collectively, HEAL research in this area hopes to help more people with low back pain do their jobs and enjoy the activities they love to do.
Find More Projects in This Research Focus Area
Explore programs and funded projects within the Clinical Research in Pain Management research focus area.
National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS)
Learn more about NIAMS’ role in the NIH HEAL Initiative.
 U.S. Department of Health & Human Services
U.S. Department of Health & Human Services
