HEALthy Brain and Child Development (HBCD) Study
Overview
The Research Need
The first few years of life are a period of exponential growth and brain development. The long-term effects of exposure to substances and other environmental, social, and biological factors during pregnancy and after birth on infant and child development are not fully understood.
To address this knowledge gap, NIH is supporting research to better understand brain and child development, beginning in the perinatal period, and extending through early childhood. Of great interest is understanding variability in brain development and how it contributes to cognitive, behavioral, social, and emotional function. Knowledge of a wide range of brain trajectories is critical to understanding how they may be affected by exposure to opioids and other substances (e.g., alcohol, tobacco, cannabis), stressors, trauma, and other significant environmental influences, including those that promote resilience.
About the Program
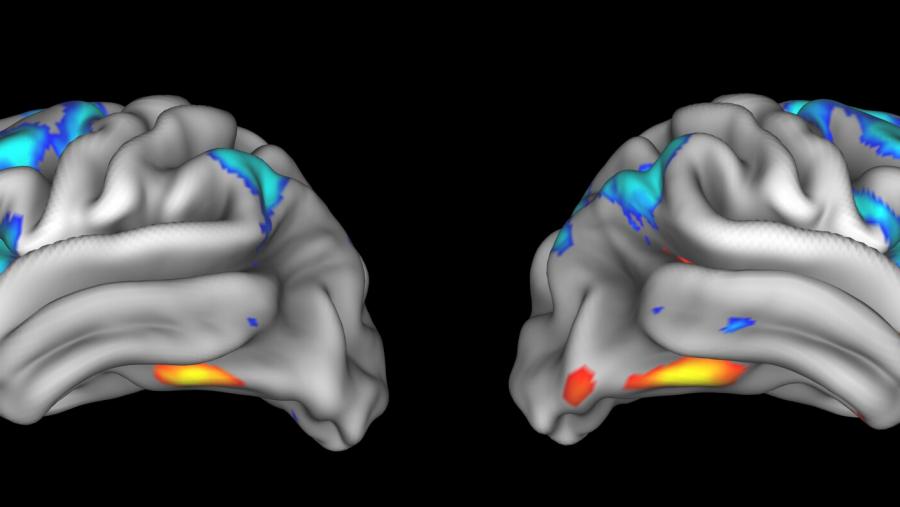
The HEALthy Brain and Child Development (HBCD) Study is the largest long-term study of early brain and child development in the United States. The study will collect information from a cohort of pregnant participants before birth and from their infants beginning at birth, and it will continue collecting information from the caregiver and child through early childhood. Data will include structural and functional brain imaging; anthropometrics; medical history; family history; biospecimens; and assessments of social, emotional, and cognitive development. Approximately half the sample will include pregnant persons who experience adversities during pregnancy including, but not limited to, exposures to substances.
Open Funding Opportunities
There are no Open Funding Opportunities at this time.
Research Examples
Examples of HBCD Study activities include:
- Multi-modal assessments of brain, cognitive, and emotional development from birth through childhood to assess neurodevelopmental trajectories and determine how substance exposure and other environmental factors affect these developmental trajectories
- Creation of a large, diverse, well-characterized cohort of caregivers, infants, and children whose anonymized data will be made available for analysis to the greater research community for years to come
- Evaluation of key developmental windows during which the impact of adverse environmental exposures (e.g., drugs, stress, COVID-19) or ameliorating factors (e.g., substance use disorder treatment, social/economic support) influence neurodevelopmental outcomes
- Identification of actionable items as results emerge that are pertinent to prevention, public policies, and innovative products
- Development, optimization, and validation of technologies for neuroimaging and neurophysiological assessments of infants, with standardized analysis pipelines
- Establishment of a collaborative research model that includes creation of community liaison boards comprising medical providers, patient advocates, ethicists, and representatives from state agencies to inform the study design and provide ongoing feedback throughout its lifetime
- Continuous assessments of child physiology through mobile and wearable technology
Upcoming and Past Events
Phase II
- Arkansas Children’s Hospital Research Institute – Arkansas
- Boston Children’s Hospital – Massachusetts
- Cedars-Sinai Medical Center – California
- Children’s Hospital of Los Angeles – California
- Children’s Hospital of Philadelphia – Pennsylvania
- Cincinnati Children’s Hospital Medical Center – Ohio
- Emory University – Georgia
- Johns Hopkins University/ Kennedy Krieger Institute – Maryland
- New York University School of Medicine – New York
- Northwestern University – Illinois
- Oklahoma State University Center for Health Sciences – Oklahoma
- Oregon Health and Science University – Oregon
- Pennsylvania State University – Pennsylvania
- University of Alabama at Birmingham – Alabama
- University of California, San Diego – California
- University of Florida – Florida
- University of Maryland – Maryland
- University of Minnesota – Minnesota
- University of New Mexico Health Sciences Center – New Mexico
- University of North Carolina Chapel Hill – North Carolina
- University of Vermont – Vermont
- University of Wisconsin-Madison – Wisconsin
- Vanderbilt University – Tennessee
- Virginia Tech - Virginia
- Washington University – Missouri
Phase I
- Arkansas Children’s Hospital Research Institute – Arkansas
- Avera McKennan Hospital & University Health Center – South Dakota
- Boston Children’s Hospital – Massachusetts
- Case Western Reserve University – Ohio
- Cedars-Sinai Medical Center – California
- Children’s Hospital of Los Angeles – California
- Children’s Hospital of Philadelphia – Pennsylvania
- Children’s Research Institute – Washington D.C.
- Cincinnati Children’s Hospital Medical Center – Ohio
- Duke University – North Carolina
- Emory University – Georgia
- Father Flanagan’s Boys’ Home – Nebraska
- Johns Hopkins University/ Kennedy Krieger Institute – Maryland
- Mt. Sinai School of Medicine – New York
- New York University School of Medicine – New York
- Northwestern University – Illinois
- Oklahoma State University Center for Health Sciences – Oklahoma
- Oregon Health & Science University – Oregon
- Pennsylvania State University – Pennsylvania
- Rhode Island Hospital – Rhode Island
- University of Alabama at Birmingham – Alabama
- University of California, San Diego – California
- University of Florida – Florida
- University of Illinois at Urbana-Champaign – Illinois
- University of Maryland – Maryland
- University of Minnesota – Minnesota
- University of New Mexico Health Sciences Center – New Mexico
- University of North Carolina, Chapel Hill – North Carolina
- University of Pennsylvania – Pennsylvania
- University of Pittsburgh – Pennsylvania
- University of Vermont – Vermont
- University of Wisconsin-Madison – Wisconsin
- Vanderbilt University – Tennessee
- Washington University – Missouri
- Women & Infants Hospital in Rhode Island – Rhode Island
Participating NIH Institutes, Centers, and Offices
- National Institute on Drug Abuse (NIDA)
- National Institute of Mental Health (NIMH)
- National Institute of Neurological Disorders and Stroke (NINDS)
- National Institute on Alcohol Abuse and Alcoholism (NIAAA)
- Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD)
- National Institute of Biomedical Imaging and Bioengineering (NIBIB)
- National Institute of Environmental Health Sciences (NIEHS)
- National Institute on Minority Health and Health Disparities (NIMHD)
- NIH Office of the Director’s Environmental influences on Child Health Outcomes (ECHO) Program
- Office of Behavioral and Social Sciences Research (OBSSR)
- Office of Research on Women’s Health (ORWH)
- National Cancer Institute (NCI)
- National Eye Institute (NEI)
Contact
Christopher Sarampote, Ph.D.
HBCD Study Project Director, NIDA
Resources
- Developmental Cognitive Neuroscience Special Issue: An Overview of the HEALthy Brain and Child Development Study - Jul 12, 2024
- HBCD Legal Analysis of Recruiting Pregnant Women Who Use Controlled Substances by State
- Legal Analysis by State Chart
- HBCD Study Technical Assistance Webinar Recording
- FAQs for HBCD Phase II NOFOs
- HBCD Maternal Neurodevelopmental and Contextual Assessments
- HBCD Service Subcommittee Report
- Risk and Resilience Special Issue
- JAMA Psychiatry Viewpoint
- HBCD PI Meeting Summary - May 4-5, 2020
- HBCD Neuroimaging Working Group Final Report
- HBCD Biospecimens Working Group Final Report
- Expert Panel Meeting on Research Methodologies to Understand Long-Term Consequences of Prenatal Opioid and Other Substance Exposure on Brain and Behavioral Development - Sep 24, 2018
- Expert Panel Meeting to Discuss Study Design for a Longitudinal Study of the Impact of Prenatal Opioid and Other Substance Exposure on Brain and Behavioral Development - Oct 12, 2018
 U.S. Department of Health & Human Services
U.S. Department of Health & Human Services